A study published by researchers from the University of North Carolina has left us shaking our heads once again. This one claims that the closer you live to a hog farm, the more likely you are to visit a hospital emergency department for a urinary tract infection.
The only problem: There’s nothing that actually proves hog farms cause urinary tract infections.
Anyone who has ever taken a statistics class has heard the phrase “correlation does not imply causation.” The concept: just because two things are true doesn’t mean they are related.
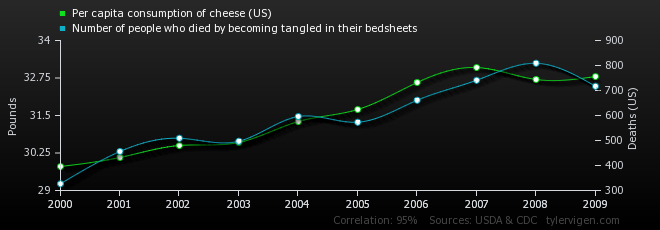
Take, for instance, the correlation between (a) per capita cheese consumption and (b) the number of people who died by becoming tangled in their bedsheets. As the chart shows, the amount of cheese we eat directly correlates with the number of people die tangled in their bedsheets — even though we all know that one does not cause the other.
This isn’t the first time we’ve encountered serious flaws with studies about our industry, including misleading claims that our farms are disproportionately located in minority communities or that hog farms are responsible for a variety of health concerns, including higher rates of asthma and higher mortality rates.
Dr. Keith Ramsey, the medical director of infectious disease control at Pitt County Memorial Hospital and former chairman of the Pitt County Board of Health, has conducted numerous clinical and research studies involving residents across eastern North Carolina. He studied health outcomes and specifically looked at possible association with bacterial resistance associated with swine operations.
His conclusion: “I have observed no indication that living near a hog farm causes any increased risk of infection by antibiotic-resistant or any other bacteria… The real health threats needing attention in eastern North Carolina are diet and lifestyle… not hog farms.”
“… The real health threats needing attention in eastern North Carolina are diet and lifestyle… not hog farms.” Dr. Keith Ramsey, medical director of infectious disease control, Pitt County Memorial Hospital
The problem with this latest study is that it doesn’t account for other factors that might cause urinary tract infections. It doesn’t explain why its data shows that American Indians are more than 90% more likely to have UTIs, why women over 65 are 139% more likely to have UTIs, or why those without private health insurance are 173% more likely to have UTIs. Do hog farms indiscriminately target these populations?
The study also doesn’t examine why so many communities across the state without any hog farms have high rates of urinary tract infections. And it doesn’t explain why communities with a high density of hog farms — and a low density of poultry farms — have a lower concentration of UTIs.
Indeed, this latest study leaves many unanswered questions, including why researchers continue to attack our state’s hog farms.
Malcolm Kendrick, the author of “Doctoring Data,” shares one potential answer: “There are many people with an agenda out there, and they will ruthlessly torture statistics until they get the answer they want out of them.”